My daughter, Olive, has always snored. A lot. She’s only six years old, but her snores rival those of a TV grandpa. But it wasn’t until I noticed that sometimes she held her breath during sleep that I started to be concerned. She’d be sleeping peacefully, then just… stop breathing. For two or three seconds. Which I know isn’t a lot of time, but when you’re watching your child, waiting for the next breath to come, it feels like an eternity.
I brought up the symptoms at our next pediatrician visit, and after a look at her throat, we learned that she had extremely large tonsils and the tell-tale signs of sleep apnea. The pediatrician said that she may need her tonsils out and recommended we see an Ear, Nose, and Throat doctor. My heart sank. I was not expecting this. A tonsillectomy was a surgery. A real operation where my daughter would be under anesthesia. A recovery where she’d be in a lot of pain. My mama brain did not want her to have to go through this.
And yet, I wanted the best thing for her, that would help her be the healthiest. So off to the ENT we went. Lo and behold, he recommended that she have both tonsils and adenoids removed. He said that removing them would eliminate the snoring and sleep apnea, and that those issues wouldn’t go away as she got older. The surgery was optional, though. Um, what?? My husband and I could choose if we wanted to do it now, or later, or not at all. How do trained medical professionals let parents decide this sort of thing?
Let me tell you, this was not an easy decision. Who wants to choose to put her child through this? How could we know for sure that we were making the right choice? Ultimately, the surgery seemed like the best way to ensure that my daughter’s breathing remained steady and didn’t cause her more problems.
We decided in April to go through with the tonsil/adenoidectomy. We scheduled it for the middle of June, but waited until school was out to tell Olive. During the ENT appointment, she had clearly been scared of the idea of having her tonsils out. She doesn’t have a great sense of time, so I thought the closer to the surgery date the better. I found a few books to help prepare her. I definitely recommend Good-Bye Tonsils! It really helped Olive understand what to expect, and though it does go a little light on what recovery will be like, I thought it did a good job of preparing without scaring. We also read Violet Mackerel’s Remarkable Recovery, which wasn’t so much about preparing Olive as it was showing someone going through this and coming out just fine on the other side. In the days leading up to surgery, we talked a lot about what it would be like. We let her pick out the ice cream, yogurt, and popsicle flavors she wanted. We chose her surgery outfit and what toy she wanted to take with her. A couple days before the surgery we had family over for pizza and “Good-Bye Tonsils” cake. She was as prepared as we could make her.
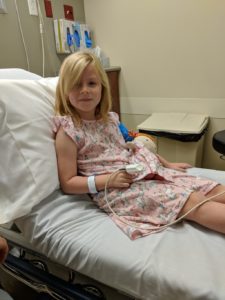
The day of surgery, we had to be at the surgery center at 6:30 a.m. Since patients can’t eat or drink after midnight, they schedule younger kids as early as possible. Olive was actually sort of excited about the surgery. Grandma gave her cute pajamas that had a matching doll pair, so Olive and her doll, Dollive (get it?), were all set. Once there, I filled out some paperwork, Olive and I got matching ID bracelets, and we waited. Before long, we went back to the pre-op area where they weighed her and took her blood pressure, and we spoke with the anesthesiologist and the surgeon. They described how things would go, and we had a chance to ask questions.
Soon it was time for them to wheel her back. I gave her a huge hug and butterfly kisses and tried not to cry too much. My husband and I went back to the waiting room. It was only about 30 minutes before we were ushered into a small room, where the doctor came in and told us that all had gone well. It was a relief, but my anxiety levels were still high since she wasn’t awake yet. We weren’t allowed to go back to see her until she was awake, so we returned to the waiting room.
Finally, we got to go back and see her. Let me tell you, this was the most difficult part. She was sobbing, clearly in distress. She moaned and her head rocked back and forth, like she was trying to escape the pain but couldn’t find a way. She was making these strange hiccupping sounds, which the nurse assured me were expected. Seeing Olive in agony made me cry. The nurse was giving me all these post-op instructions but all I wanted to focus on was Olive. Why can’t they give you the instructions during some of the waiting time? As soon as they removed her blood pressure cuff, and she had gone through all the fluid in her IV bag, they removed the IV (the tape removal literally made her scream) and we could go home. I thought we’d want to stay awhile to make sure she was doing OK, but she just kept repeating how much she wanted to go home. I wanted nothing more than to do that for her. I couldn’t take away her pain, but I could take her home.

So at 9:45 a.m. we were in the car and headed home, officially entering the recovery stage of the journey. The first day was rough. She cried off and on all day, and had a lot of trouble swallowing. She barely slept, even though everyone told us the pain medication would knock her out. Her face was pale, and she had fierce red marks around one eye and around her jawline. I assume it was related to having her mouth held open wide during the procedure? Thankfully those marks faded by Day 2. Each day she got a little better, but there were lots of ups and downs along the way. Every night for the first several days was AWFUL. She woke a lot, crying in pain. Her whole body would shake from the anxiety over swallowing. She’s not normally a kid who overreacts to pain, so her reactions were especially difficult to watch. I expected that she would sleep in our bed for one night, but she spent the first six nights there because she woke so frequently.
Her favorite recovery foods were ice cream (surprise, surprise), yogurt, popsicles, and applesauce. It took four days before she attempted anything that required chewing, and then only took a few small bites. Sneezing and coughing were painful, as was brushing teeth. She didn’t like opening her mouth too wide, and at times wouldn’t even talk. We watched a lot of Netflix, read a lot of books, and played a lot on the tablet.

Olive’s eight-year-old brother was a little bit enormously jealous. Jealous of the attention and all the ice cream, jealous of the cards Olive received in the mail, jealous that she got to sleep in Mommy and Daddy’s bed. He repeatedly told me that he wanted his tonsils out, too. I had arranged several playdates for him and overnights with grandparents to keep him busy and let Olive rest. He was entertained, but also felt like he wasn’t allowed to be at home. There was just no winning, but we tried the very best we could.
Many things about this process were not what I expected. I hope that if your child needs a tonsillectomy, this blog will give you one more perspective on what the process is like. At the time of this writing, Olive is only seven days post-op. I cannot wait until she is completely healed and back to feeling good.
















